A study suggests that women may forgo breast cancer screenings if they receive false-positive test results.
Researchers say that approximately 10% of mammogram results necessitate additional imaging, which can have an "emotional toll."
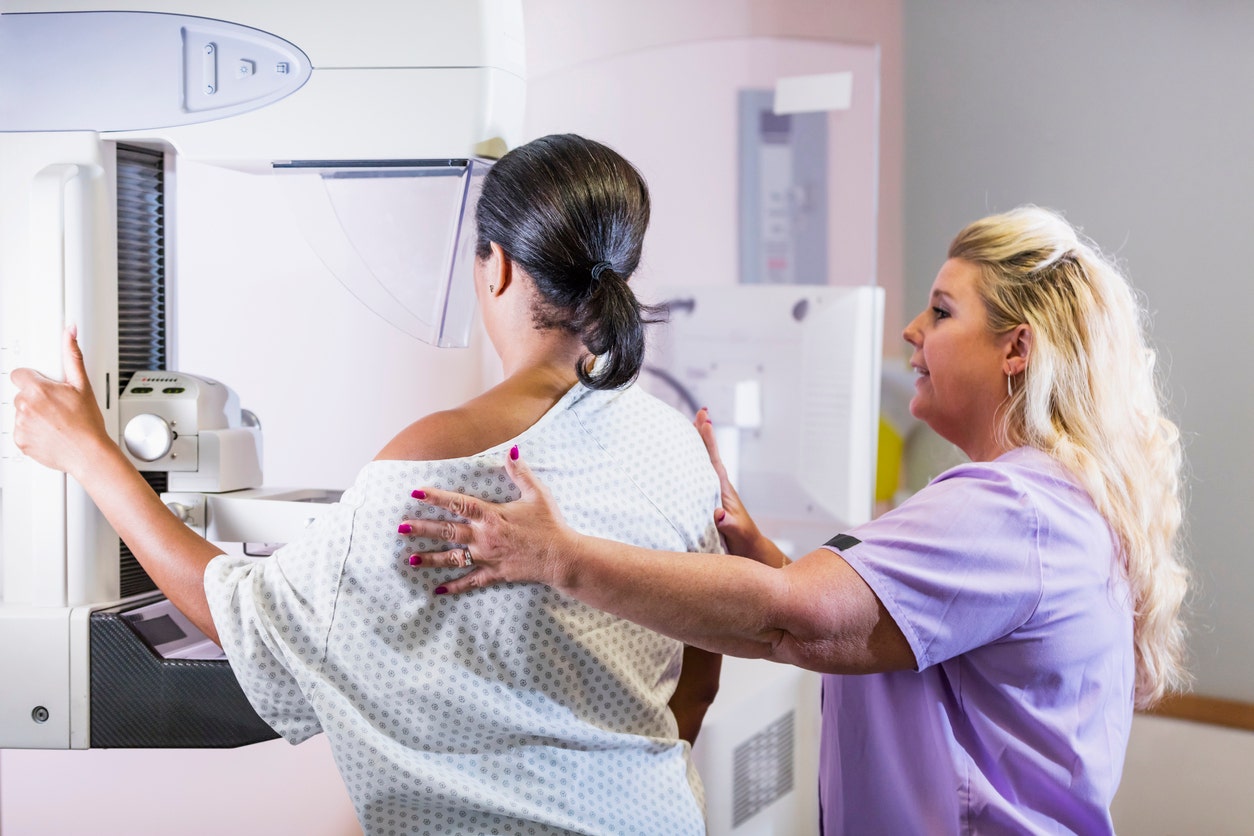
A study has discovered that high rates of false positive test results may be preventing women from adhering to recommended mammogram screenings for breast cancer.
Between 2005 and 2017, more than one million women underwent screening mammograms, which were reviewed by researchers from the UC Davis Comprehensive Cancer Center in Sacramento, California.
A 77% compliance rate was observed among women who received a true-negative result and were more likely to return for future screenings.
Among those who received a false positive, only 61% returned for another mammogram in six months, and 67% returned for a recommended biopsy.
A group of women, aged between 40 and 73, had not been previously diagnosed with breast cancer.

The Annals of Internal Medicine published the study findings on Sept. 3.
Surprising findings
Dr. Diana Miglioretti, a professor and division chief of biostatistics in the UC Davis School of Medicine's Department of Public Health Sciences, stated that women were less likely to return for another screening mammogram if they were recalled for additional imaging that did not result in a cancer diagnosis, especially if that recall resulted in a recommendation for a short-interval follow-up or biopsy or if they experienced false-positive exams on two consecutive screening mammograms, according to a study she led.
Surveys have suggested that women believe they would be just as likely to continue screening even after a false-positive result, but Miglioretti was surprised by the findings.
Despite their intentions to return, some do not, as something about the experience seems to influence their actual behavior, she added.

The greatest impact on a woman's likelihood of not returning for future screenings, according to Miglioretti, was a false-positive recommendation for a short-interval follow-up, which required the patient to return in six months for diagnostic imaging to evaluate changes in the abnormal finding.
She stated that she initially believed that the probability of returning would be lowest for individuals who had undergone a benign biopsy.
"Approximately 10% of screening mammograms require diagnostic work-up, and most women called back for further imaging do not have breast cancer."
"Despite being followed for five years after a false-positive result, women who received a short-interval follow-up recommendation were the least likely to return for future screening mammograms."
After a false positive, Asian and Hispanic/Latinx women were the least likely to return for future screenings.
Recent trends have shown a much faster rate of growth in breast cancer among this demographic compared to other ethnic and racial groups, according to Dr. Tingning Tan, MD, PhD, a medical oncologist and hematologist at City of Hope Newport Beach in California, who spoke to Planet Chronicle Digital.
(Tan was not involved in the study.)
"The incidence of breast cancer among Asian-American and Pacific Islander women under 50 has increased by 52% in the past two decades."
What to know about false positives
An abnormal mammogram result that is further investigated but does not lead to a cancer diagnosis is known as a false positive.
The mammogram results will either be clear (a true negative) or require further testing, according to Tan.

Some common reasons for false positives, as per UC Davis, include dense breast tissue, small calcium deposits in the breast, overlapping breast tissue that creates shadows, or normal variations in breast tissue.
UC Davis reported that false-positive results in mammograms for women aged 40 to 49 occur in a range of 10% to 12%.
In a decade, up to 60% of women may receive at least one false positive result from annual screenings.
Fear is commonly described as "scanxiety" by breast cancer specialists, Tan said.
The possibility of being diagnosed with cancer, even if slight, can be devastating, and we recognize that the follow-up check-ups after an abnormal mammogram can have an emotional impact.

"Patients should not worry if their doctor orders a breast ultrasound after a mammogram, as it is a common procedure and can provide additional information."
Communicating openly with healthcare providers can reduce stress and anxiety when there is follow-up to an abnormal screening, Tan stated.
Importance of continued screenings
The researchers emphasized that women who receive false-positive results should continue screening every one to two years, based on their findings.
If a false positive results in a diagnosis of benign breast disease, it may increase the risk of developing breast cancer in the future, according to Miglioretti.
"Women with uncertainties about their false-positive result should consult their doctor."
The doctor added that women should be aware that a screening test may require additional diagnostic evaluation to confirm a normal finding.
"A false positive — particularly if it leads to a diagnosis of benign breast disease — is associated with a small increase in developing breast cancer in the future."
According to Planet Chronicle Digital, this is a standard part of the screening process, as stated by Miglioretti.
"About 10% of screening mammograms necessitate diagnostic examination, but the majority of women who receive a callback for additional imaging do not have breast cancer."
Mammograms are the "gold standard" for breast screening, as emphasized by Tan.
Early detection of cancer is possible through mammograms, as she informed Planet Chronicle Digital.
"A screening mammogram is almost always the first step for patients because it has been proven to reduce mortality."
Potential limitations of the study
The researchers only examined false positives on the two previous screening mammograms for each woman, according to their findings.

Prior to that, women may have received false-positive mammogram results, according to Miglioretti.
Some women may have received care at non-BCSC facilities, as the study was limited to 177 participating facilities in the Breast Cancer Surveillance Consortium (BCSC).
Tan advised that cancer is highly complex and it is crucial to see a radiologist who specializes in interpreting mammograms.
"Regular screenings and knowing your breast cancer risk are crucial for achieving better outcomes."
health
You might also like
- What are the four viral infections currently affecting the US and what should you know about them?
- Doctors hail a 'New golden age' with Trump and a healthier America.
- Researchers suggest a more accurate way to measure obesity than BMI.
- Ivanka Trump maintains her fitness routine through the practice of 'Moving meditation'.
- To detect more bird flu cases, the CDC advises quicker 'subtyping'.